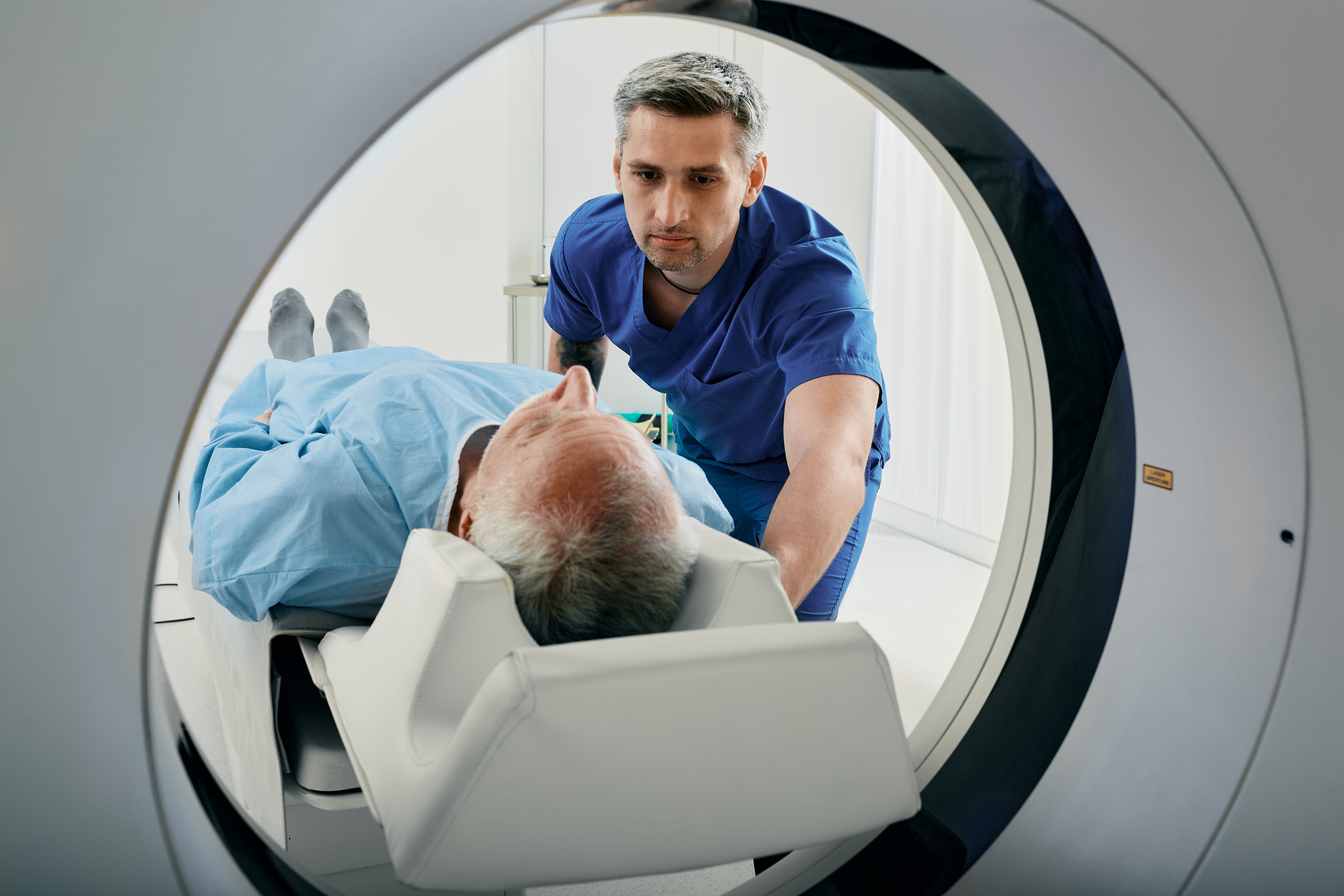
Then at the age of 75 I started my first biologic, the anti TNF etanercept. No luck so I moved to adalimumab a few months down the line. I still had symptoms and it was hard to know what was age related and what was related to active inflammation.
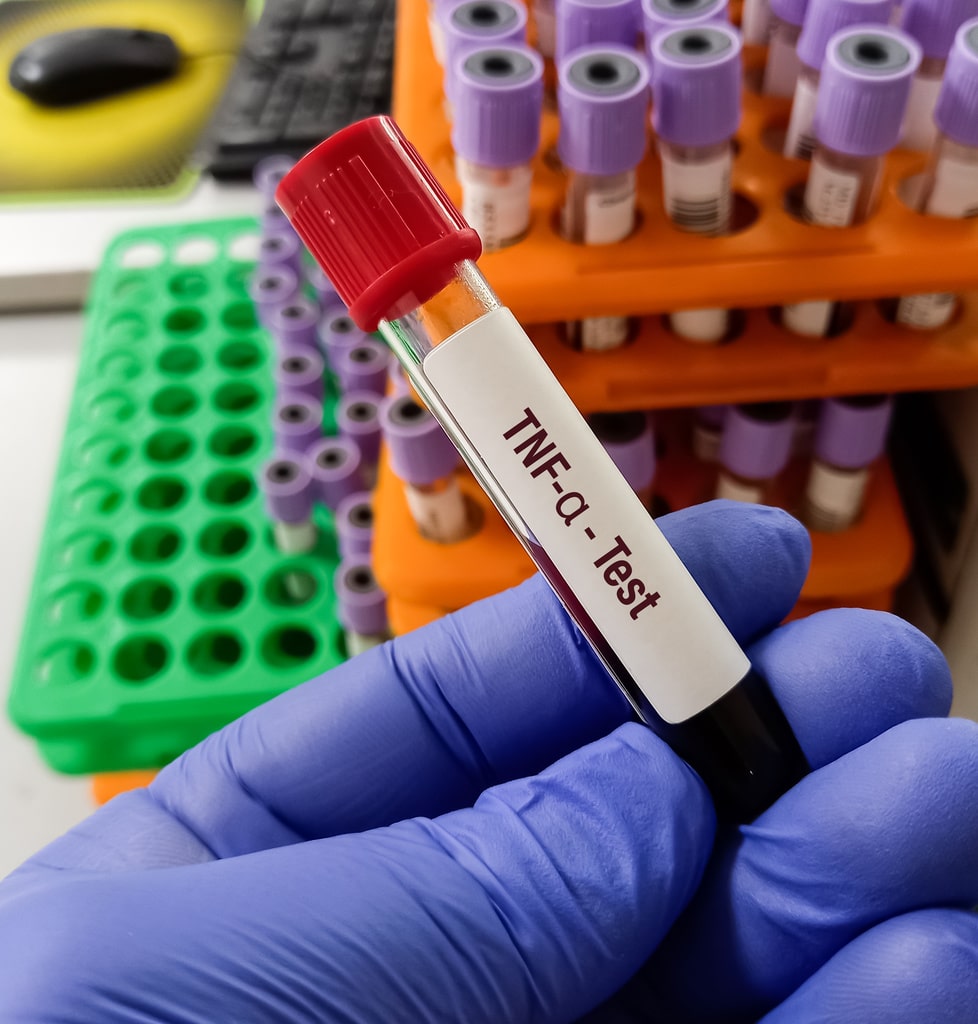
At this point I was referred on to another rheumatology department and they suggested trying the anti IL 17A secukinumab. At 77 I finally found a treatment that changed my life! The effect was remarkable and my back pain and enthesitis (when Inflammation occurs at the site where ligaments or tendons attach to the bone) were finally resolved. I will be 84 soon and am delighted to report it’s continued working. During the time being on biologics I have not experienced the immuno-suppressive risk that comes with them, with just a single infective episode of bursitis.
This rheumatology department also offered a remarkable opportunity – a two-week rehabilitation course with a group of other people with axial SpA. My time at the Royal National Hospital for Rheumatic diseases included medical check-ups, including blood tests and scans, talks from specialist nurses, occupational and physio-therapy assessment, daily physiotherapy and hydrotherapy, and psychological support. A real bonus was comparing notes about our experiences, with people of different ages and backgrounds in the group.
The course is still running and I can’t recommend it highly enough.
We still need to remind doctors of the possibility of axial SpA in younger people with back pain and suggestive symptoms, particularly if there is a family history, and a positive genetic test. My story, and the very late onset, and then benefit of specific treatment, are obviously a very rare example of axial SpA, but do suggest that a diagnosis of axial SpA should be considered at any age, if there has been a history of back pain which has come and gone over the years. It’s just so easily missed or put down to other causes.