Act on axial SpA: A Gold Standard time to diagnosis
The current time to diagnosis of axial SpA in the UK averages approximately 8.5 years from symptom onset. This delay is unacceptable and has serious consequences for the patient. With our act on Axial SpA campaign, we propose a roadmap for reducing the time from symptom onset to diagnosis to just one year. This is a call for support, to act on Axial SpA.
Rationale
Axial spondyloarthritis (axial SpA) is a life-long inflammatory condition that primarily affects the spine and sacroiliac joints. Axial SpA is more common than people realise, affecting 1 in 200 adults in the UK, which is more than the number of people with multiple sclerosis and Parkinson’s disease combined (1, 2).
The current time to diagnosis of axial SpA in the UK averages approximately 8.5 years from symptom onset (4). This delay is unacceptable and has serious consequences for the patient.
Diagnostic delay is associated with:
- Less favourable response to treatment and worse outcomes in disease activity, quality of life, fatigue, function, spinal mobility and radiographic damage to the spine (3, 5-7)
- Difficulty sleeping and higher prevalence of mental health and psychosomatic disorders (7)
- Increased likelihood of work disability, unemployment, job loss and higher healthcare costs (3)
One study demonstrated impaired spinal mobility to be twice as high in people with a diagnostic delay of over six years, in comparison to those diagnosed in less than six years (3).
Calling Time on Delay – A Gold Standard Approach
With our act on Axial SpA campaign, NASS propose a roadmap for reducing the time from symptom onset to diagnosis of axial SpA in the UK from 8.5 years, to just one year.
Karl Gaffney is Professor of Rheumatology at Norwich, Clinical Lead for Axial Spondyloarthritis and Clinic Trials Director. He is also Chair of the Medical Advisory Board at NASS. In the above video, Professor Gaffney introduces the concept of the NASS Gold Standard Time to Diagnosis programme, and the importance of collaboration between primary and secondary care in its implementation.
The patient journey to diagnosis: sources of delay in axial SpA
In collaboration with Professor Karl Gaffney and Dr Raj Sengupta, NASS have identified four broad sources of delayed diagnosis, from a ‘follow-the-patient’ perspective. Our proposals for addressing these delays have been informed by a scoping literature review and national consultation process; receiving unanimous support from 202 key stakeholders for a gold standard time of one year from symptom onset to diagnosis of axial SpA. These stakeholders included people living with axial SpA, healthcare professionals, professional bodies, communications experts and commissioners.
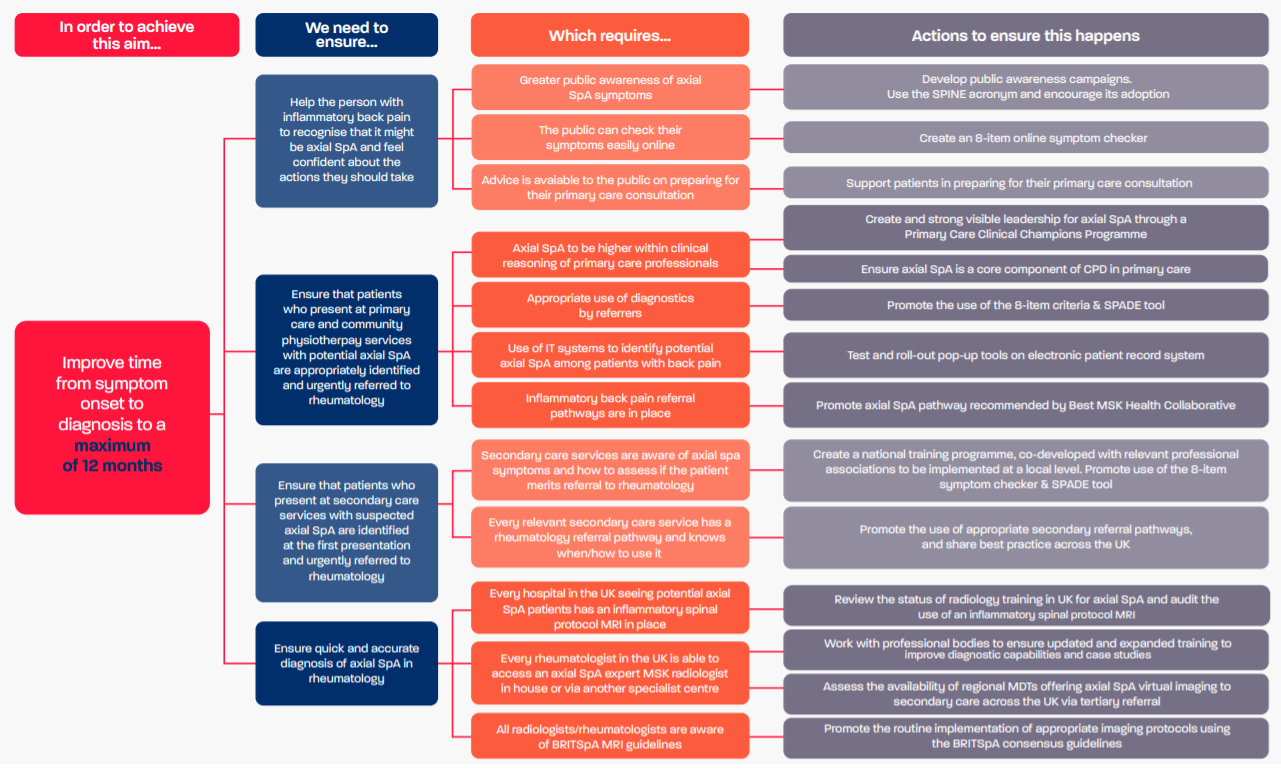
The 4 delays and our proposed vision for reducing delay to diagnosis in axial SpA are detailed in the figure below, with greater detail and evidence base provided in our signature Act on Axial SpA: A Gold Standard Time to Diagnosis document.
References
1. Hamilton L, Macgregor A, Toms A, Warmington V, Pinch E, Gaffney K. The prevalence of axial spondyloarthritis in the UK: a cross-sectional cohort study. BMC Musculoskelet Disord. 2015;16.
2. Facts and Figures | National Axial Spondyloarthritis Society 2019 [Available from: https://nass.co.uk/about-axial-spondyloarthritis/as-facts-and-figures/].
3. Yi E, Ahuja A, Rajput T, George AT, Park Y. Clinical, Economic, and Humanistic Burden Associated With Delayed Diagnosis of Axial Spondyloarthritis: A Systematic Review. Rheumatology and Therapy. 2020.
4. Sykes MP, Doll H, Sengupta R, Gaffney K. Delay to diagnosis in axial spondyloarthritis: are we improving in the UK? Rheumatology. 2015;54(12):2283-4.
5. Seo MR, Baek HL, Yoon HH, Ryu HJ, Choi HJ, Baek HJ, et al. Delayed diagnosis is linked to worse outcomes and unfavourable treatment responses in patients with axial spondyloarthritis. Clin Rheumatol. 2015;34(8):1397-405.
6. Sieper J, van der Heijde D, Dougados M, Mease PJ, Maksymowych WP, Brown MA, et al. Efficacy and safety of adalimumab in patients with non-radiographic axial spondyloarthritis: results of a randomised placebo-controlled trial (ABILITY-1). Ann Rheum Dis. 2013;72(6):815-22.
7. Ogdie A, Benjamin Nowell W, Reynolds R, Gavigan K, Venkatachalam S, de la Cruz M, et al. Real-World Patient Experience on the Path to Diagnosis of Ankylosing Spondylitis. Rheumatol Ther. 2019;6(2):255-67.
